Also See: Resources for Robotic Surgery
Dr. Christopher Pohlman, a physician at Boulder Community Hospital in Colorado, specializes in minimally invasive surgery, operating through tiny openings in his patients. But those incisions aren’t always done with a traditional scalpel by hand, with Pohlman hovering over the body when the cuts, exploration and surgical repair are done inside his patients.

Photo: Boulder Community Hospital
Dr. Christopher Pohlman, a physician at Boulder Community Hospital in Colorado, specializes in minimally invasive surgery, operating through tiny openings in his patients.Rather, his second-hand man — or in this case, machine — does the work while Pohlman guides the robotic “hands” from a high-tech console nearby. The hardest part of doing general surgery with a robot is positioning the patient, Pohlman told The Washington Diplomat. The robot’s four long instrument-like arms stretching down from its towering body have to be placed just so. “It’s like docking a space station.”
This outer-space sight is becoming more and more common in surgery rooms nationwide as robotic-assisted surgery becomes standard practice for certain procedures. And more often than not, that mechanically artistic precision is courtesy of the da Vinci Surgical System, by far the most widely used robotic system around. In the span of just over a decade, da Vinci brand robots are now being used at more than 1,000 hospitals and clinics around the country for a variety of surgeries ranging from gynecological disorders to heart bypass to gallbladder removal to prostate and other types of cancer.
The robots’ every move is watched and guided by surgeons like Pohlman. In a typical surgery, Pohlman makes three to six puncture wounds called “ports” and then threads a miniature camera into one of them so that what’s happening inside the patient shows up on nearby video screens. Pohlman performs these surgeries weekly, some with and some without the help of the hospital’s da Vinci robot. He also does traditional “open” operations with larger incisions, including hernia repairs “not suited to the robot.”
When the da Vinci is on duty, Pohlman sits at a console a few feet from his patient with a virtual-reality, three-dimensional screen magnifying whatever images the camera picks up. He controls the robot’s arms and the surgical tools at their tips with joystick handgrips. A computer eliminates normal human hand tremors, making his moves more precise and, as he described it, “more elegant.”
Such minimally invasive surgeries have been shown to cause significantly lower blood loss and reduce the likelihood of infection, according to Kim Capps, head surgical nurse and manager of robotic surgery at Boulder Community Hospital. “With a prostatectomy or a hysterectomy, patients used to lose 600 milliliters [about 20 ounces] of blood. With robotic surgery it’s a tablespoon,” she said. “And because the openings are the size of two dimes, robotic surgeries reduce the chance of infection.”
Almost all surgical robots around the globe are da Vinci models developed and sold by a California company, Intuitive Surgical Inc. However, while surgical robots can offer many benefits, including less pain for the patient and faster recovery times, “the robot is a tool, not an end all. Just because the technology is there, it doesn’t mean it’s always best,” Pohlman cautioned.
For example, a da Vinci robot makes Pohlman’s operations on an esophagus or a stomach valve easier to do. It’s “a snap” to correct gastroesophageal reflux disease now, he said. Still, the da Vinci is of questionable benefit for certain surgeries such as removing a tumor on the pancreas. It can also be problematic for some patients, including those who have scar tissue from previous procedures.
Maryland cardiac surgeon Dr. Johannes Bonatti similarly underscored that all surgeries, especially complex ones, carry risks of complications and death — and studies show robotic surgeries have about the same complication rates as other types of surgery. Bonatti is a professor at the University of Maryland School of Medicine in Baltimore and a recognized innovator in robotically assisted heart procedures.
Another downside to the da Vinci is sheer cost — each system runs upward of $1 million, with more than $1,000 worth of parts needing replacement after each procedure and lengthy training times for surgeons to become proficient in using the robot.
But that hasn’t deterred da Vinci’s stunning rise in the medical market. As Bonatti himself put it: “There’s an excitement in my field right now, as heart surgery becomes more and more precise, less destructive, and more patient friendly with the help of robots.”
Dr. Elisa Trowbridge, a reconstructive surgeon and assistant professor of obstetrics and gynecology with the University of Virginia Health System in Charlottesville, agrees. She points out that “these days, you can’t be a gynecologist and a surgeon without robotic training. Top-notch physicians are expected to know about it.”

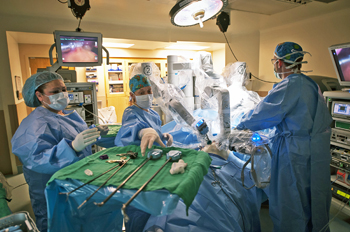
Photo: Boulder Community Hospital
During robotic-assisted surgery, the surgeons “operate” from a high-tech console near the patient using joystick handgrips to guide every move of the robots’ hands while watching images of what’s happening inside the patient’s body on a virtual-reality, three-dimensional screen.The Food and Drug Administration approved the da Vinci robot for surgery in the United States only 11 years ago, although the first da Vinci-assisted surgeries were already being done in Belgium (on gallbladders) and Germany (prostate). Yet by last December, 1,676 da Vinci systems were installed in more than 1,500 hospitals worldwide.
This impressive upsurge was influenced by early adopters in the United States who brought the system into the medical mainstream, according to Intuitive Surgical Senior Marketing Director Christopher Simmonds. He noted that U.S. surgeons have driven robotic developments in the fields of urology and gynecology while general surgery has been most strongly influenced by advances in South Korea.
The international footprint is clearly growing. Intuitive notes that Malaysia and India, for instance, have four da Vinci robot systems each, while Germany has about 50 and Britain nearly 30.
Interestingly, surgical robots and “tele-surgery” were developed in the 1980s at the former Stanford Research Institute, now SRI International, funded by the U.S. military for possible battlefield use. Intuitive Surgical was a 1995 commercial spin-off. For obvious reasons, remote off-site surgery continues to attract attention from the Department of Defense and NASA.
The expansion of robotic surgery varies according to particular specialties, with prostate surgery the most frequently performed robotic procedure worldwide.
Prostate cancer, in fact, gave birth to the practical application of robots in medicine. Dr. Mani Menon, director of the Vattikuti Urology Institute at Henry Ford Hospital in Detroit introduced the use of robotic surgery to remove a cancerous prostate gland back in 2000. Since then, he’s become a leader in the field, performing thousands of robotic-assisted surgeries. Menon was a protégé of Johns Hopkins University’s Dr. Patrick Walsh, who pioneered a new approach to prostate surgery that kept patients from becoming impotent and incontinent after the procedure by sparing delicate nerves in the prostate. Despite the innovation, Walsh still relied on a surgeon’s hands to physically explore the patient’s pelvis area.
Menon’s robot changed all that, and da Vincis are now used in about half of all prostate surgeries in the United States.
That also means that prostate cancer provides some of the best-documented results for the robots’ performance. This March, a major study at Henry Ford involving 3,000 patients found that “robot-assisted surgery to remove cancerous prostate glands is safe over the long term, with a major complication rate of less than 1 percent.”
One reason why robotic prostate surgery took off when robots entered the scene, many experts say, is that open prostate surgery can be unwieldy and difficult. It involves an awkward location and tiny nerves that directly affect continence and potency. As a result, it had a lot of complications and unhappy patients, even if they were cured of the cancer that brought them to the operating table. Most studies have confirmed that robotic surgery for prostate cancer is effective in eliminating or controlling the cancer while preserving sexual function and continence.
Robotic prostate surgery is now a mature discipline with “enough well-trained people” to produce consistently good outcomes, said another founding father in the field, Dr. William D. Steers, chair of the Urology Department at the University of Virginia Health System in Charlottesville who is also president of the American Board of Urology and has performed hundreds of robotic prostatectomies.
When the FDA gave robotic surgery a green light in 2000, Steers went to the robotic prostate pioneers at Henry Ford, took a sabbatical to learn their techniques, then brought Ford folks back to Virginia to help set up a similar program there. “Prostate surgery is humbling because it’s so complex,” he told The Diplomat. “You have to preserve microscopic nerves” that control urinary and sexual functions. Steers recognized right away that the visual detail and magnification of a da Vinci system and the computer-aided hand control enable surgeons to do precisely that.
The advantages of the robot are similar for a chest surgeon operating on the lungs, according to Dr. Keith Mortman, a thoracic surgeon at Washington Hospital Center in D.C. Although Mortman, named one of Washingtonian magazine’s “top doctors” last year, has been a surgeon for 12 years, robotics are a relatively new tool for him.
“I was a skeptic,” he admitted. “But I started watching fellow surgeons doing it and the benefits are real.”
Among them he noticed reduced blood loss; with cancer patients, the visual magnification allowed for a more complete surgery; there were “fewer air leaks” in lungs, a common complication; and with chest surgeries where some areas are difficult to see, the robots offered “superior visualization,” Mortman said.
But for all their benefits, robotic surgeries have real risks — and real critics.
The lack of tactile feedback with the robot means “everything is visual,” Pohlman pointed out. “That can be dangerous. You have to make sure to keep all instruments in view” and have well-trained surgical assistants.
A more general problem is that all minimally invasive and laparoscopic surgeries, including the robotic ones, have a steep learning curve. And there are plenty of detractors who maintain that a machine simply can never mimic the “touch” that an experienced doctor has cultivated over years of work. Indeed, with a robot, the lack of physical feedback means that a surgeon’s brain has to do without that highly honed sense of touch, relying only on the visuals the robot provides.
But just as a blind person’s brain can develop a “sense of hearing,” Steers of the American Board of Urology says a robotic surgeon will eventually learn to get tactile or “haptic” (a sense of touch) information from the visual input, as the brain translates sight cues into touch signals. The key, however, is practice, practice and practice.
Another difficulty is overly high patient expectations fueled by optimistic anecdotes and sleek advertising. Robotic surgery may be precise, but it’s not perfect, and there are no guarantees that prostate patients who had a robot operate on them won’t experience the same post-surgery problems as those who didn’t. Robotic surgery tends to speed up recovery times, but likewise, there are plenty of exceptions and each case is individual.
There’s also the concern that the trend toward robotics is needlessly pushing the procedure on patients without regard to cost or benefit, a worry that’s especially acute among prostate patients. A recent article in the New York Times by Gina Kolata for instance detailed the pressures that patients exert on physicians to provide them with a robotic surgery that promises less pain and shorter recoveries. The desire is only natural — hospitals readily promote these benefits. And with da Vinci systems costing anywhere between $1 million and $2.3 million, hospitals have a strong financial incentive to make sure they get used. That in turn may be pushing some surgeons into robot-aided procedures before they’re ready.
But there are simple ways for patients to protect themselves and find an excellent surgeon, experts advise.
First, unless there’s a truly compelling reason to try an experimental procedure or use an inexperienced surgeon, you want someone who’s had all that practice, practice, and practice.
How much is enough? Exact numbers may not always be the best guide, but generally, “you want someone who operates every week” with a robot, says Trowbridge of the University of Virginia Health System. She believes that most surgeons need at least 100 surgeries to reach a very good performance level — and even more for complex procedures.
Likewise, Steers recommends against any physicians who perform only a handful of robotic surgeries a year, although “some low-volume facilities and surgeons do well.” However, because prostate surgery is one of the most complex procedures, he recommends someone with case experience “in the hundreds” for prostate patients.
Bonatti of the University of Maryland Medical School also agrees that “high volume produces quality,” advising that patients should also consider the quality not just of the surgeon, but of the entire operating team. He said the best way for a surgeon to learn minimally invasive surgery is a fellowship that lasts one or two years.
Pohlman had a yearlong fellowship in laparoscopic techniques and robotic surgery, during which time he was practicing and learning all day long under an experienced mentor. The shift from open to laparoscopic surgery is “the most difficult,” he said, but once you master it, “moving to the robot is easy.”
For his part, Mortman did a fellowship in minimally invasive chest surgery and shadowed expert practitioners. He advises patients to ask for robotic-related numbers, including hospital frequencies, because higher volumes of robotic surgery are indicative of more experienced surgeons and staff.
Future surgeons are now trained three ways, Trowbridge explained: on inanimate objects, on lab animals, and on virtual trainers. “The future of training is digital,” she noted.
Steers believes the best robotic-surgery training takes place when there’s a da Vinci double console that lets the student and mentor work in tandem, but that’s an expensive approach. “My bias? Everybody should do a sabbatical in robotic surgery,” he said.
Looking to the future, Steers said robotic surgery would be well served if it had more “centers of excellence” all around the country. These would generate better outcomes across the board. He also believes better data needs to be collected through more multinational clinical trials, national repositories and tighter reporting standards.
But the future is, to some degree, already here — with robots taking over where human hands have left off. My own recent experience perhaps offers a glimpse into a revolutionary field whose future remains positive overall, but not perfect.
A trip to the emergency room for what I thought was food poisoning had actually left me a candidate for gallbladder removal with the option of using a da Vinci surgical robot. After consulting with Pohlman on the advantages and disadvantages, I decided to give Dr. da Vinci a try.
The gallbladder removal went as planned and two hours later, a bit light-headed, I was home again. The next morning I took a Tylenol, got up, and made breakfast for my family.
But within weeks I joined the ranks of patients who expect too much from robots, dismayed that I lacked my old energy. At the end of the day, whether the cuts were made by metallic or human hands, I still had major surgery and had to cope with the trauma of that surgery, minimally invasive or not. I will never know if the stress would have been greater with a more invasive procedure. Whatever the case, who would have thought that a simple gallbladder removal could represent a shiny bold new frontier in surgery.
In the Washington area, robotic surgery procedures are performed at various hospitals, including:
George Washington University Hospital in Washington, D.C.
www.gwhospital.com/Hospital-Services-O-Z/Robotic-Surgery
Johns Hopkins Medicine in Baltimore, Md.
www.hopkinsmedicine.org/surgery/about/innovations/min_invasive_robotic.html
Suburban Hospital in Bethesda, Md.
www.suburbanhospital.org/Robotics/RoboticsOverview.aspx
Inova Health System hospitals in Virginia
www.inova.org/healthcare-services/surgical-services/types-of-surgical-procedures/da-vinci/index.jsp
University of Maryland Medical Center
https://www.umm.edu/robotics/
About the Author
Carolyn Cosmos is a contributing writer for The Washington Diplomat.

